Spring 2026 - Vol. 21, No. 1
PHOTO QUIZ FROM THE PRIMARY CARE ADVANCED PRACTICE PROVIDER ONBOARDING PROGRAM
A Common Complaint, An Uncommon Cause
Kerri Schlicher, MSN, CRNP, FNP-C
Nurse Practitioner, Family Medicine Strasburg
Penn Medicine Lancaster General Health Physicians
CASE HISTORY
A 59-year-old female presents to the clinic with persistent left leg swelling that started about two-and-a-half months ago. She describes a feeling of tightness, some redness that started about four weeks ago, a sensation of burning that has been disrupting her sleep, as well as numbness and tingling in her left foot and toes. The patient reports no recent injury or trauma to the area. She denies any recent extended immobilization.
After trying some interventions and discovering that use of ice and elevation provided only temporary relief, she consulted a physician from a different health system about two weeks ago. She reports that an ultrasound was completed and that although no blood clots were found, there were some slightly swollen lymph nodes. She was told to use ibuprofen and elevate the leg.
Despite trying these, she feels the condition is worsening. A further review reveals no chest pain, fever, or shortness of breath.
She had varicose vein surgery on the right leg 12 years ago but reports that the veins in her left leg were “not too bad.” She also reports a history of cellulitis in the right leg a few years ago that was treated with prednisone. She has no history of blood clots.
The patient has not been seen in her primary care office for over 10 years. She is not currently on any medication and has no other significant past medical history.
On examination, she is in no distress and has normal vital signs. There are no open areas or wounds present. The swelling is localized to her lower extremity, with no swelling noted above the knee. Fig. 1 shows the initial presentation of the patient’s swollen left leg.
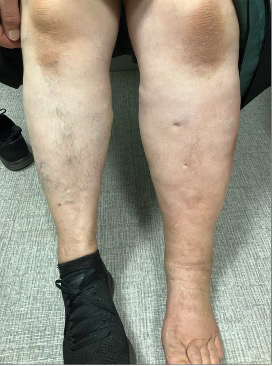
Fig. 1. Left lower leg edema compared to the right leg.
The left lower leg is warm and tender to touch with 3+ pitting edema and erythema. No swelling is present in the patient’s left foot or above the knee. She has a negative Homan’s sign, and her pedal pulses are 2+ bilaterally. The patient’s lungs are clear, and she exhibits no other signs of fluid overload.
At the time she leaves the office, she is treated for cellulitis with amoxicillin 875 mg twice daily for one week. She is also advised to continue elevating the leg and start using compression stockings during the day when she is on her feet. A repeat ultrasound is ordered to rule out a deep vein thrombosis (DVT).
The ultrasound shows no evidence of an acute left lower extremity DVT; however, pathologic left inguinal lymph nodes measuring up to 4.2 cm are noted. Further imaging with a pelvic ultrasound is recommended in the next one to three months to determine the cause of her lymphadenopathy, and tissue sampling is recommended if she has persistent lymphadenopathy.
One week later, the patient follows up in the office. She reports no change in her symptoms with the use of amoxicillin. Her assessment is also unchanged. She is prescribed cephalexin 500 mg twice daily for seven days to see if additional microbial coverage would be any more effective. She is encouraged to continue elevation and compression use. Due to the lack of response and the enlarged lymph nodes, a computed tomography (CT) scan of the patient’s abdomen and pelvis and a chest X-ray are ordered for further evaluation.
QUESTIONS
- What are some possible causes of lower extremity edema?
- What are the risk factors for DVT?
- What are possible causes of inguinal lymphadenopathy?
ANSWERS
- Possible causes of lower extremity edema include, but are not limited to, varicose veins, chronic kidney disease, cirrhosis, DVT, chronic venous insufficiency, heart failure, cellulitis, lymphedema, medication side effects, and malignancy involving lymph nodes leading to obstruction.1
- Some risk factors for DVT include male gender, a recent hospitalization or extended period of immobilization, congestive heart failure, trauma or fracture, soft tissue injury, infection, varicose veins, clotting disorders, smoking, pregnancy, acute malignant neoplasm, and use of hormonal contraception.2
- Inguinal lymphadenopathy can be caused by sexually transmitted infections, localized skin and soft tissue infections, and other viral or bacterial infections. Less common but serious causes of lymphadenopathy include lymphoma and metastatic disease.3
ADDITIONAL CASE HISTORY
When the additional imaging is completed, the chest X-ray shows large pulmonary nodules consistent with metastases (see Fig. 2).

Fig. 2. Chest X-ray showing multiple lung nodules bilaterally.
The CT of the patient’s abdomen and pelvis shows large enhancing left inguinal lymph nodes without other findings of intra-abdominal metastatic disease. The radiology service concludes that based on the location and distribution of her disease, the cause is likely a malignancy in the lower extremity such as melanoma or sarcoma. When the patient returns to the office to reassess her lower extremity edema, the imaging is reviewed and the patient is notified of the findings.
An urgent referral is placed to the oncology service. In the meantime, a needle biopsy of the lymph node and a chest CT are ordered, as well as an MRI of the brain.
The needle biopsy reveals a high-grade, poorly differentiated malignant neoplasm. The differential diagnosis at this time includes melanoma, primitive neuroectodermal tumor (PNET), and a poorly differentiated carcinoma with neuroendocrine differentiation. Malignant melanoma seems most likely.
The lymph node and the lung nodules are presumed to be metastases, and the original site of the assumed melanoma is not identified. The brain MRI shows a few tiny but concerning foci of enhancement in brain parenchyma, suggestive of early intracranial metastatic disease.
DISCUSSION
Unilateral lower extremity edema can be caused by many different pathologies as discussed above. In this case, the patient’s leg swelling was not a result of cellulitis but an underlying melanoma leading to metastasis. Prompt imaging and close follow-up helped identify the cause of the patient’s swelling and guide the next steps in the treatment plan to set the patient up for the best possible outcomes.
In the United States in 2024, there were an estimated 100,640 new cases of cutaneous melanoma.
4 Melanoma of unknown primary (MUP) accounts for approximately 2% to 4% of all melanoma cases in the nation. MUP is believed to arise when there is regression of a known primary site, likely driven by immune responses involving T cells and natural killer cells.
Molecular studies suggest that MUP likely comes from the skin, as it often has the pattern of ultraviolet (UV) damage mutations found in cutaneous melanoma. Other melanoma types, such those originating in mucosal or uveal locations, have different mutation patterns and lack UV signatures.
5
Clinical evidence also supports this theory, as patients with MUP often have vitiligo and regressed pigmented lesions, as well as a higher prevalence of dysplastic nevi compared to the general population. MUP is thought to most commonly originate from areas on the trunk and lower limbs.
5
Lymph node involvement is the most common presentation in patients with MUP, with axillary and inguinal nodes being the most frequently affected areas. In a study of MUP patients, 65% presented with lymph node metastases only, especially the axillary, groin, and cervical locations. A minority of MUP cases present with visceral metastases (25%), brain involvement (16%), or skin/subcutaneous lesions (10%).
6
Clinical signs to look for include a history of previously excised skin lesions without histological examination, vitiligo, or regressed pigmented lesions, which may suggest immune-mediated regression. A complete skin exam should be performed, with attention paid to evidence of regressing lesions.
MUP tends to affect men more often than women, and most cases appear in patients between the ages of 40 and 60 years. Based on lymphatic drainage patterns, the trunk and lower limbs are considered the most likely sites of primary disease, so it is important to focus on these when completing the skin exam.
CASE OUTCOME
The patient was seen promptly by the oncology service and started on chemotherapy. Discussion about starting radiation for more targeted therapy of metastases also occurred, but the decision was made to repeat imaging after a few rounds of chemotherapy to determine response.
The patient had a hard time tolerating chemotherapy, with the biggest complication being severe diarrhea. She was hospitalized for other complications including colitis and a small bowel obstruction. She is currently on a break from chemotherapy due to these complications. The patient’s prognosis at this time remains unclear.
REFERENCES
1. Goyal A, Singh B, Afzal M. Peripheral edema. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; April 5, 2025.
https://www.ncbi.nlm.nih.gov/books/NBK554452/
2. Chopard R, Albertsen IE, Piazza G. Diagnosis and treatment of lower extremity venous thromboembolism: a review.
JAMA. 2020;324(17):1765-1776.
3. Falk N, Joseph R, Dieujuste M. Lymphadenopathy: evaluation and differential diagnosis.
Am Fam Physician. 2025;112(3):286-293.
4. Sundararajan S, Thida AM, Yadlapati S, et al. Metastatic melanoma. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; February 17, 2024.
https://www.ncbi.nlm.nih.gov/books/NBK470358/
5. Bossio S, Rassy E, Samartzis E, et al. Melanoma of unknown primary: new perspectives for an old story.
Crit Rev Oncol Hematol. 2021;158:103208.
6. Anbari KK, Schuchter LM, Bucky LP, et al. Melanoma of unknown primary site: presentation, treatment, and prognosis — a single institution study. University of Pennsylvania Pigmented Lesion Study Group.
Cancer. 1997;79(9):1816-1821