INTRODUCTION
Trauma care is a major public health problem, and injury remains the neglected disease of the 21st century. Among children and young adults aged 1-34, unintentional injuries, homicide and suicide are the first, second and third leading causes of death respectively.1 More lives of persons aged 1-34 are lost to injury than to all other causes of death combined. Accidents are the second leading cause of years of potential life lost, after heart disease.2 Trauma care is extremely expensive and poses a significant economic burden on our health care system. Other less easily measured effects that trauma inflicts on society are the pain, grief, family and societal disruption and psychological effects of disfigurement, as well as long-term disability from such traumatic conditions as burns, severe head injury, spinal cord injury, amputations, etc. Despite the staggering societal costs, trauma-related research has been chronically underfunded. The total 2008 NIH budget allocation for traumatic injury research was $308 million, while for cancer research it was $5.6 billion, and for HIV/AIDS it was $2.9 billion.3 This monograph will trace the history of trauma system development in the United States; describe the different levels of trauma care; review the benefits they provide in terms of lives saved; and describe the trauma center at Lancaster General Health and what it means to our community.
HISTORICAL PERSPECTIVE OF TRAUMA SYSTEM DEVELOPMENT IN THE U.S.
Many of the early advances in care of the injured patient can be attributed to lessons learned in the major military conflicts of the U.S. during the 20th and 21st centuries. World War I introduced the concept of evacuation from the battlefield, and World War II brought blood transfusion and resuscitative fluids. In Vietnam, battlefield mortality was further reduced by having medics at the point of wounding who were more highly trained, and by prompt aero-medical evacuation. The Iraqi theatre conflicts have seen further refinements of trauma surgery with the reintroduction of tourniquets, the Forward Surgical Station, and the use of damage control techniques to avoid physiological depletion prior to definitive care.4
Civilian care was slow to adopt the advances in trauma care that derived from our military conflicts. In 1966, the National Academy of Sciences National Research Committee on Shock and Trauma published its “white” paper, “Accidental Death and Disability: The Neglected Disease of Modern Society.” 5 This document highlighted the enormity of the problems of dealing with trauma care in the U.S., as well as the lack of proper facilities (trauma centers), and set forth recommendations for their development. In 1976, the Trauma Committee of the American College of Surgeons published “Optimal Hospital Resource for Care of the Seriously Injured.” 6 This document, which is updated every three years, describes personnel and equipment requirements that a trauma center must have, and described a tiered capability in Level I, II and III, trauma centers. This document’s 1976 description of a trauma care system as an integrated continuum all the way from accident prevention through rehabilitation, including everything in between, is still true today. Likewise, trauma care is largely a team effort, involving a substantial commitment, not only of institutional infrastructure, but also of personnel. Not only must capable personnel be immediately available at all times (thus requiring trauma surgeons to be “in-house”), there must also be sophisticated hospital services that can provide tertiary and quaternary care 24/7/ 365. The “optimal care” document sets out explicit requirements for Level I, II and III (and now IV) trauma centers. The Trauma Committee of the American College of Surgeons (ASCOT) sends out experienced trauma surgeons to do vigorous 2-day site surveys for hospitals to be verified as a Level I, II, or III trauma center. If the hospital meets the criteria for a trauma center, it can proudly wear that imprimatur for three years until it must undergo an entirely new verification from scratch. Some states such as Pennsylvania choose to self-designate, but the requirements are similar to those of ASCOT or are even more rigorous.
DIFFERENCES BETWEEN LEVEL I, II AND III TRAUMA CENTERS
Level I trauma centers represent the highest level of capability and are regional resource centers that usually serve population-dense areas. They are expected to be able to manage a high volume of the most severely injured trauma patients. There is invariably a 24-hour in-house attending trauma surgeon and 4th and 5th year surgical residents as adjuncts. The Level I conducts original research and is a leader in education, prevention and outreach activities.
A Level II trauma center incorporates many (>90%) of the same requirements as a Level I, but differs mainly in not needing the essential requirement for research, a surgical residency, and a certain annual volume of patients. In certain situations, requirements may allow surgeons in Level II centers to take call from outside the hospital if they can be present at the patient’s beside within a specified interval in response to certain physiologic derangements.
Level III trauma centers have continuous general surgical coverage, which may consist of certified general surgeons or trauma surgeons. The general surgeon must be available for all major resuscitations and should be capable of managing some less severely injured patients at the home facility. They would have a close working relationship with a nearby Level I or II center, along with explicit transfer agreements.
Level IV trauma centers are a relatively new designation. Level IV’s usually occur in rural settings and may involve smaller critical access hospitals that may not even have a general surgeon on staff. Level IV facilities provide initial assessment and stabilization of injured patients prior to transfer to a Level I or II center for definitive care. Few, if any, trauma patients are cared for directly at Level IV trauma centers.
ARE TRAUMA CENTERS BENEFICIAL?
The answer to that question is most certainly “yes,” as has been demonstrated by improved outcomes in numerous studies in many different locales. McConnell, et al7 in a retrospective study of 542 patients with head injury in Oregon and Washington noted that when patients were transferred from rural trauma centers to Level I trauma centers, there was a 10.1% (95% CI: 0.3% - 22.2%) reduction in mortality. Clancy, et al8 analyzed trauma registry data from the North Carolina registry database to determine if there were differences in outcome between Level I vs. Level II trauma centers for more severe injuries (aortic disruptions, liver injuries, pelvic fractures and pulmonary contusions). Using multiple logistic regression analysis and controlling for Revised Trauma Score, Injury Severity Score, age, gender and race, they found there was no difference between Level I and Level II trauma centers.
MacKenzie, et al9 compared mortality among patients in 14 states treated either in a Level I trauma center (18 hospitals), or in a hospital without a trauma center (51 hospitals). Using propensity scoring to adjust for differences in case mix, the mortality rate was significantly lower at trauma centers than at non-trauma centers (7.6% vs. 9.5%; relative risk 0.80; 95% CI 0.66 to 0.98). The authors of this seminal study concluded that the risk of death is significantly lower when care is provided in a trauma center, and this argues for continued efforts toward regionalization. It should be noted that the small (though significant) difference in outcome between non-trauma centers and trauma centers in MacKenzie’s 2006 study may reflect the vast overall improvement in trauma care during the years from the original 1965 ‘white paper.’ Specifically, courses like Advanced Trauma Life Support and Pre-hospital Advanced Trauma Life Support, have significantly improved the care of the trauma patient, even for the non-trauma center. Demetriades, et al, 10 using the National Trauma Databank in over 130,154 patients, examined the adjusted mortality for Level I vs. II trauma centers and found that in patients who are more severely injured (Injury Severity Score >15), the mortality was notably higher in Level II trauma centers vs. Level I (odds ratio 1.14, CI 1.09 to 1.20; p<0.0001).
Hass, et al11 examined the process of care that leads to improved survival at designated trauma centers. Time from admission to relevant interventions was assessed in hypotensive penetrating trauma (PT) and blunt traumatic brain injury (TBI) with mass effect. For both types of injuries there was a survival advantage at trauma centers vs. non-trauma centers even though there was no significant difference between median times to radiographic assessment or operative intervention. From this study, the authors concluded that the improved outcome at trauma centers was not a result of more rapid assessment and intervention, and the factors that contribute to the survival benefit of trauma center care are more complex.
LANCASTER GENERAL LEVEL II TRAUMA CENTER
If trauma centers have such a demonstrable benefit on survival, why are there fewer than 450 Level I or Level II trauma centers in the nation’s 6,000 hospitals? Two reasons account for this circumstance: commitment and resources. Commitment by a hospital to trauma care must be 24/7, which means that when a major trauma victim presents, the hospital’s resources are focused on providing that patient’s care, sometimes to the exclusion of other patients. For instance, a patient with a gunshot wound to the abdomen sustained in a drug deal that went badly has first priority in the operating room over all previously scheduled elective operations. Needless to say, this can be quite disruptive to the smooth ebb and flow of hospital services, and many hospitals don’t want to experience that disruption.
Further, a trauma center must have an immediately available trauma team of expert trauma surgeons, trauma nurses, specialty surgeons (such as orthopedic traumatologists and neurosurgeons), ED physicians, anesthesiologists, and other subspecialty support. The potential for sudden physiologic deterioration of the trauma patient requires many of these physicians and specialists to be “in-house” at night, because trauma is mostly a nocturnal disease. These same specialists who take call through the night face the prospect of a full day of elective surgery the next day with little to no sleep. Many physicians find this a major source of dissatisfaction in their careers and choose not to participate in trauma call. Lack of commitment of physicians to participate in the trauma call roster is forcing many trauma centers to give up their Level I or II status.12
Financing is also a major factor in a hospital’s decision to become a trauma center as most hospitals don’t find trauma to be a profitable enterprise. The severity adjusted national average for per patient costs in trauma care in 2003 was $14,869.13 Total trauma center costs in 2003 were $10.1 billion, and total trauma center loss was estimated at $1 billion. In the increasingly hostile climate of medical care reimbursement by the government and 3rd party payers, many hospitals are making the difficult decision to opt out of developing a trauma center when faced with the fiscal reality of doing so.
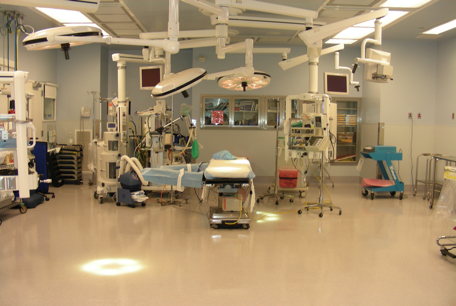
Fig. 1: Lancaster General Hospital Trauma OR
The Lancaster community is extremely fortunate that Lancaster General Health (LGH) has both the commitment and resources necessary for the Trauma Service to provide excellent care to the trauma patients of Lancaster County and its surrounding area. This commitment is demonstrated by the fact that LGH was one of the first hospitals in the state of Pennsylvania to be designated by the Pennsylvania Trauma Systems Foundation (PTSF) in 1986, and since that time has taken care of over 23,000 trauma patients.
Physicians, nurses and administrators at LGH have taken leadership positions on the PTSF, including the highest level, the Board of Trustees. LGH surgeons have pioneered the use of ultrasound in the evaluation of blunt abdominal trauma.14 In terms of resources, the administration of LGH has delivered both the hardware (facility) and software (components), maintaining the highest level of capacity and capability of the trauma program. The hardware additions include a state-of-the-art dedicated trauma OR with over 730 square feet that opened in December 2009 (Figure 1), equipped with digital image technology and heart bypass capability. The layout was designed for flexibility and to allow more than one surgical procedure to be done concurrently. In addition, in 2008 LGH built a dedicated state-of-the-art 16-bed trauma ICU. The software additions include the recent hiring of six board-certified trauma/critical care physicians, trained at some of the finest trauma fellowship programs in the country. All have a broad range of trauma, critical care, general surgery and research experience.
The mainstay of any trauma program is its Performance Improvement (PI) program. Pennsylvania mandates that all verified trauma centers send detailed quarterly reports to the state on all complications and mortalities. Our four trauma case managers collect all complications concurrently on daily rounds, which are entered into a detailed statewide database by our expert trauma registrars. Seminal morbidities and all mortalities are discussed on a monthly basis at our Trauma Morbidity and Mortality Conference to look for opportunities to improve our care. Our trauma PI program has been noted to be a major strength of our trauma center on our accreditation visits with the PTSF. Lancaster General Health’s trauma morbidity and mortality figures compare quite favorably with other trauma centers across the state of Pennsylvania. In 2009, compared with all other Level I and II trauma centers in the state, LGH had lower overall complication rates in 18 of 23 complication audit filters used by the American College of Surgeons, and 14 of those 18 were significantly lower. Also, our overall unadjusted mortality rate for trauma was lower than the statewide mortality rate in all other trauma centers.
SUMMARY
Trauma centers save lives, but they require an intense commitment of both personnel and facilities to maintain the rigorous standards set forth by the PTSF. LGH and the community it serves are fortunate to have an outstanding Level II trauma center that can provide care for the trauma patient from Genesis to Exodus (prehospital → rehab). We who work in the trauma arena are excited that we are on the cusp of some great changes in the LGH trauma center in the years ahead. With our evidenced-based approach and the rigorous use of protocol-driven care we hope to see further reductions in our mortality rate. In addition, we hope the clinical research we perform will keep us on the cutting edge of further improvements in trauma care. Finally, we look forward to educating the next generation of trauma surgeons as Lancaster General Hospital expands its programs of medical education.
REFERENCES
1. National Center for Health Statistic Data. Accessed May 6, 2010. Internet web site: http://www.cdc.gov/ncipc/wisgars
2. Haenszel W. Standardized rates for mortality defined in units of lost years of life. American Journal of Public Health 1950;40:17-26.
3. NIH Estimates of Funding for Various Research, Condition, and Disease Categories (RCDC). Accessed May 6, 2010. Internet web site: http://report.nih.gov/rcdc/categories.2009.
4. Schwab CW: Crises and War: Stepping Stones to the Future. Journal of Trauma 62(1):1-16, 2007.
5. Accidental Death and Disability: The Neglected Disease of Modern Society. Washington, DC, Division of Medical Sciences, National Academy of Sciences, National Research Council, September 1966.
6. Optimal Hospital Resources for Care of the Seriously Injured. American College of Surgery Bulletin 61(8):6 August 1976.
7. McConnell JK, Newgard CD, Mullins RJ, et al: Mortality Benefit of Transfer to Level I vs. Level II Trauma Centers for head-injured patients. HISR: Health Services Research 40(2):435-457 (2005).
8. Clancy TV, Maxwell G, Covington, DL, et al: A Statewide Analysis of Level I and II Trauma Centers for Patients with Major Injuries. Journal of Trauma; 51:346-351, 2001.
9. MacKenzie EJ, Rivera FP, Jurkovich GJ, et al: A National Evaluation of the Effect of Trauma Center Care on Mortality. NEJM; 354:366-378, 2006.
10. Demetriades D, Martin M, Salim A, et al: The Relationship Between American College of Surgeons Trauma Center Designation and Mortality in Patients with Severe Injury (Injury Severity Score >15. J. American College of Surgeons 202:212-215, 2006.
11. Hass B, Jurkovich GJ, Wang J, et al: Survival Advantage in Trauma Centers: Expeditious Intervention or Experience. J. American College of Surgeons 208:28-36, 2009.
12. Esposito TJ, Maier RV, Rivera FP, et al: Why Trauma Centers Prefer Not to Care for Trauma Patients. Archives Surgery 126:292-297, 1991.
13. National Trauma Foundation for Trauma Care “US Trauma Center Economic Status” 2003. www.traumacare.com/download/NFTC_crisisreport_May2004.pdf (accessed May 13, 2010
14. Jarowenko D, Hess R, Herr MS, et al: Use of Ultrasonography in the Evaluation of Blunt Abdominal Trauma. Journal of Trauma; 29(7):1031, 1989