 Click to Print Adobe PDF
Click to Print Adobe PDF
Winter 2011 - Vol.6, No.4
|
When the East Meets the Amish:
An Application of Folk Medicine in the Amish Community
Yuri Anna Lee
Student Nurse Extern, Lancaster General Health
Lisa A. Ruth-Sahd RN, DEd, CEN, CCRN
Extern Faculty Coordinator, Lancaster General Health
|
  |
Some of the earliest memories of my Korean childhood involve the aromatic scent of distilling herbs bubbling away in a glass pot, the smell clinging like a second identity to my clothes and hair. A child does not think much about the significance of such home remedies, only that it is an integral part of life. I was jarred into realizing that it was not the “norm” when other kids in my class crinkled their noses as I walked by, as if they caught a whiff of my foreignness and not the smell of the earth’s essence. When they came for a sleepover, their horrified eyes expressed what they thought about the never-ending rows of bowls and little plates of roots and vegetables that were to be eaten with rice, as much for their taste as their healing properties. I desperately wished then that they were macaroni and cheese, hamburgers, and mashed potatoes. Little did I realize that such familiarity with the comforting properties of various leaves and roots, so generously provided by the earth and lovingly prepared by my traditional Korean grandmother, would stand me in good stead as a nursing student.
Burdock, also known as Love Leaves,1,2 was just one of those many herbs that were among the regulars in our house. The roots were eaten and the leaves were dried and made into tea. Our culture is so closely intertwined with that of the Chinese and Japanese that the Korean nation for many centuries used Chinese characters for writing until a Korean emperor came up with his own. To this day, most of the elders can read some Chinese. Due to the Japanese occupation of Korea, most of those same elders can also speak some Japanese, as they had been forced to forget their native tongue and speak that of the occupier. This close sharing of history as well as close geography provides us collectively as Asians with some similar customs, including a past steeped in the use of herbs, both as medicine and as food.
As a nursing extern, I recently had the opportunity to care for an Amish patient who had suffered a traumatic farm accident. “Samuel” is a 44-year-old farmer whose horse had been spooked, causing him to be dragged for 50 feet by the 5000-pound machinery. He suffered a displaced fracture of the left fibula, a fracture of the right fibula and posterior femoral condyle with a torn meniscus, as well as multiple abrasions, contusions and lacerations of both legs. He was hemodynamically stable and underwent an incision and drainage procedure for a 7 cm laceration on the right knee and placement of a knee immobilizer.
Samuel and his wife “Sadie” were both very pleasant, but quiet and distant. When addressed they were polite and were very appreciative of any care provided, but did not make clear eye contact. Their body language was wary. One of their requests caused concern among the nurses on the floor, whose seeming indifference to that request put up some barriers between the patient and the nursing staff. It seemed that Samuel wanted to use “burlap” leaves to help control his pain. As a member of his care team, I was very confused. What were “burlap” leaves? No one seemed to know. The nurses were very hesitant to ask. The staff had had a prior experience with such leaves in the care of another critically injured Amish patient and that situation had left a negative impression. They were understandably very concerned about any substance that could cause infection if placed on the incision site or on skin abrasions. Samuel and his wife were told that the attending physician would have to be consulted on the use of any alternative treatments.
When the physician rounded, she confirmed that the leaves posed no harm and could be applied while the patient was in bed to help alleviate the patient’s pain. Since no one else seemed to know anything about the leaves, I went into the room, introduced myself and told the patient and his wife that the doctor had cleared the use of the leaves. When asked what type of leaves they were, the wife answered that they were Burdock leaves. I nodded and said I was familiar with Burdock and that in my Korean culture, it was used extensively, both medicinally and as a delicacy. Sadie stared. Samuel stared. And then the smiling began. I stated that in Chinese medicine Burdock had been used for centuries for its cleansing effects on the kidneys and liver, as well as topically on the skin to cure rashes. Asians, I explained, felt Burdock was very valuable as an antibacterial and antiseptic. I had grown up drinking it as a tea and eating the roots. They stared some more. Samuel’s jaw was ajar and his wife just kept smiling at me.
Sadie explained that they were new to the use of Burdock leaves and “didn’t know people used them internally.” The elders of their ordnung had recommended them and obtained organically grown and dried leaves for their use. I asked how the Amish community used the leaves and she explained “they are steeped in boiling water, much like tea. The leaves are blanched into softness, but not cooked by the heat, then squeezed out and placed in a double layer on the skin.” This procedure is felt to be effective in drawing out pain and promoting healing. I suggested that since a physical therapist was going to come in soon, perhaps they would like to wait until after that, at which time I would be happy to help facilitate the treatment. In the meantime, they were happy to hear that I would provide them with printed information from the Internet on the internal uses of Burdock, and would provide information about Burdock leaves to the care team to help facilitate treatment when I was not there.
Later, when a nurse’s aide provided the couple with a basin of hot tap water that left Sadie dissatisfied because the water was not quite hot enough to effectively steep the leaves, I boiled water in the microwave and offered to help by steeping the leaves and squeezing out the water so Sadie could apply them more efficiently.
She was quite pleased with this arrangement, and while we worked together, Samuel and Sadie asked me how old I was, if I were married and had children. They shared that they had nine children themselves and had recently had their first grandchild. When we were finished applying the leaves, Sadie pulled a piece of paper out of her purse to show me what her daughter had written to comfort her father while he was in the hospital. Clearly, the couple had metamorphosed from being guarded to being open and willing communicators. I was able to reason with them about the inadvisability of their plan to place the leaves under the immobilizer as this could possibly cause blisters or sores on the leg. They agreed the leaves would only be applied when the brace was not on. I strongly sensed that they were willing to comply with the instructions because they knew their wishes were not being ignored and their beliefs were being respected. Sadie stated how heartwarming it was to meet someone who wanted to understand their Amish culture and who demonstrated love of neighbor.
At the end of their stay on the floor, just before discharge, the couple thanked me profusely, and “Samuel” said quietly, “You know, you’re alright.” I felt that was the most rewarding endorsement he could give me. This is what it means to be a nurse – to connect with your patient, build trust so that they realize you care about them and want to meet their needs, whether physical, emotional or spiritual. This experience underscores the fact that as a nurse I never want to view the cultural mores or spiritual beliefs of a patient as evidence of their “foreignness” but as facets of who they are as individuals. Those facets are what make people shine and make them unique. It is our responsibility as nurses to find out what those facets are and help them shine brilliantly.
BURDOCK LEAVES
Burdock is any of a group of biennial thistles in the genus Arctium lappa, family Asteraceae and seem to grow just about anywhere in the world.3,4 Plants of the genus Arctium have dark green oval leaves up to 71 cm. long on a stalk that may grow to a height of 80-150 cm. They have a coarse, woolly underside and lower leaves on the plant resemble a heart (Fig. 1). Arctium species flower from July through to October and is considered to be an invasive species in North America. Other names for Burdock include: Bardana, Burr Seed, Cocklebur, Hareburr, Love Leaves, Personata, Philanthropium, and Thorny Burr. The pharmacological compounds in Burdock are reported to include small amounts of volatile oils such as phenylacetylaldehyde, benzylaldehyde; lignans such as neoarchtiin; caffeic acid derivatives, polysaccharides, and phytosterols,3,4 though it is safe to assume that none of these is unique to this plant.
Fig. 1. Burdock Plant.
 Fig. 1. Burdock Heath-shaped Leaf.
Fig. 1. Burdock Heath-shaped Leaf.
 Fig. 1. Flower of Burdock.
Fig. 1. Flower of Burdock.

Uses for Burdock
The taproot of young Burdock plants can be harvested and eaten as a root vegetable in a variety of dishes that are popular in Asia, particularly Japan and Korea.1,3,4 Immature flower stalks may be harvested in late spring before flowers appear. Their taste resembles artichoke, to which the Burdock is related.
In the second half of the 20th century, due to the increasing popularity of the macrobiotic diet, Burdock achieved international recognition for culinary use. It contains a fair amount of dietary fiber (GDF, 6g per 100g), calcium, potassium, amino acids,1,3,4 and is low in calories.
Traditional Herbal Medicine
Burdock is a traditional medicinal herb used for many ailments, and is a common component of traditional Chinese medicines. Folk herbalists consider dried Burdock to be antibacterial, antineoplastic, antioxidant,5 antiretroviral, and anti-inflammatory,6,7 and they feel it also has hepatotprotective properties.8,9 Burdock root oil extract, also called Bur oil, is popular in Europe as a scalp treatment applied to improve hair strength, shine and body, help reverse scalp conditions such as dandruff, and combat hair loss. Burdock root oil extract is reportedly rich in phytosterols and essential fatty acids (including rare long-chain EFAs),9,10,11 the nutrients required to maintain a healthy scalp and promote natural hair growth. However, minoxidil is the only topical treatment that has been shown to improve hair growth in controlled studies.
An Innovative Burn Treatment
Burdock leaves are described by alternative medicine practitioners as very helpful in the care of burns, especially for pain management.12 Users report that it eases dressing changes and appears to impede bacterial growth on the wound site by promoting a moisture barrier. In individual cases, Burdock is claimed to shorten healing time, prevent the need for skin grafts, and reduce scarring.
According to a Christian alternative medicine website,12 Burdock was introduced into the care of burns by John Keim, an Amish alternative practitioner, who was in dire need of a remedy to treat his son’s burns. Having gone to the woods to meditate and seek Divine guidance, his attention was drawn to big plantain leaves which he believed would serve as an ideal non-stick barrier between the salve he had applied to his son’s body and the gauze body wrap. After using various types of leaves, Burdock became his treatment of choice because of the size and availability of the leaves.
Fig. 2. "Samuel" receiving a Burdock leaf treatment.
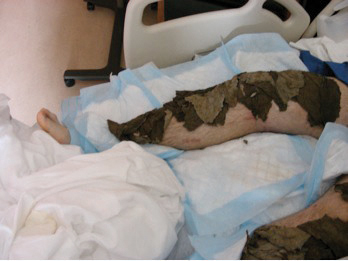
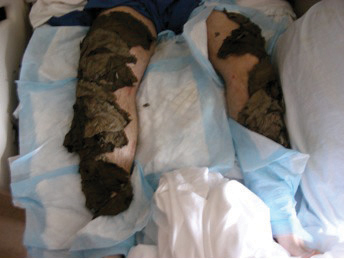
How Burdock Leaves are Used
Burdock leaves are harvested when they are a bit larger than a man’s hand. They are dried in a warm, dark place for 4-7 days. They are stored in a plastic tub with a tight lid until needed, at which time they are rehydrated with boiling water.
Hospitals focusing on holistic care13 include the use of Burdock leaves in the treatment of wounds and burns. Burdock leaves work nicely to cover large burned areas. Holistic healthcare providers have reported the ability to change dressings with limited morphine or pain management. These same purported healing benefits account for its use for deep as well as superficial leg wounds or broken bones as in the case reported here (Fig. 2), though a mechanism of action would be hard to explain in such cases.
IMPLICATIONS FOR HEALTH CARE PROVIDERS
Madeline Leininger’s theory of nursing care, called transcultural nursing, addresses the influence of cultural considerations on a nurse’s relationship with the patient.14,15 High quality nursing care should harmonize with the cultural beliefs, practices, and values of the people we serve in our community.14,15 As a second semester nursing student, I had instinctively applied the tenets of culturally congruent care.
One of the theory’s tenets is cultural accommodation or negotiation, which refers to “creative nursing actions that help people of a particular culture adapt to or negotiate with others in the health care community in an effort to attain the shared goal of an optimal health outcome for client(s) of a designated culture.”14 A related tenet of trans-cultural nursing theory acknowledges the various dimensions of cultural and social structure, and encourages identifying “factors related to religion, social structure, …cultural values, and ethno-history that influence cultural responses of human beings...”14,15 To fulfill this tenet I first needed to find out exactly what the patient’s cultural needs were and what they expected of me as their nursing care provider in fulfilling those needs.
As nurses, we need to keep in mind that “culture care concepts have both different and similar aspects among all cultures of the world.”16 In my situation, the Amish custom of folk remedies and my own Asian background of Chinese herbs blended together to make a beneficial healthcare experience for my patient. Nurses need to be quick to use their own life experiences and personal knowledge to relate to others, focusing on similarities rather than on differences.
Most cultures have folk remedies. In order to provide holistic and culturally congruent care, the culturally sensitive nurse is sensitive to such traditions if a client introduces them. Such nursing care is beneficial, healthy, culturally satisfying and enhances the well-being of our patients.3 This is an essential nursing concern, one that can help nurses increase their knowledge of and demonstrate their respect and appreciation for cultural diversity. The technical explanation of Leininger’s theory of transcultural nursing14 can be summed up simply in a universal tenet that the Amish community lives by…love thy neighbor.
In order to serve the Amish community in Lancaster County with cultural competence, we must recognize that folk medicine persists in the Amish culture because it has been secluded from mainstream society. In earlier times Amish communities did not have easy access to physicians. In times of illness they resourcefully used common cures at hand, or remedies handed down through the generations.4 To the Amish community, old ways are desirable, even preferred, and the advice of an elder person, especially concerning medical treatment, carries more weight than the advice of a scientifically educated person.16 Some Amish still practice Powwowing, an Old World brand of faith healing.16 An awareness that many of the Amish believe the cause of illnesses to be rooted in sin5 and that they are suspicious of higher learning in general,16 can help a nurse to understand why a patient may refuse or be noncompliant with treatments and preventive medicine. Such realizations can help prevent a judgmental attitude that would only foster conflict.
A PERSONAL REFLECTION
This experience touched my heart deeply. Samuel and Sadie felt that I had a sincere desire to connect with them, and consequently they felt cared for and they reciprocated positively. The Amish live by the precept of love of God and of neighbor; the fact that they felt I had shared neighborly “love” with them makes me feel honored. I have learned that something as innocuous as the Burdock leaf can become the foundation for a therapeutically successful nurse-patient relationship that results in an extraordinary experience for the patient. These Love Leaves will become my symbol for providing an extraordinary experience every time I have contact with a patient; a symbol of love for the cultural diversity that makes life in our community meaningful and enjoyable.
Resources
1. Gruenwald, J. Brendler, T. Jaenicke, C. (Eds.). (2007). PDR for herbal medicines (4th ed.). Montvale, NJ: Thompson Healthcare Inc. >
2. Hostetler, J. (1964). Folk and scientific medicine in Amish society. Human Organization; 22(4): 269-275. >
3. http://www.efloras.org/florataxon.aspx?flora_id=1&taxon_id=20706. ^ a b "Arctium". Flora of North America. >
4. http://www.efloras.org/florataxon.aspx?flora_id=1&taxon_id=102484. Retrieved 2011-07-05. >
5. Predes, FS. Ruiz, AL. Carvalho, JE. Foglio, MA. Dolder, H. (2011). Antioxidative and in vitro antiproliferative activity of Arctium lappa root extracts. Complementary and Alternative Medicine; 239(11): 25. >
6. Sohn, E-H. Jang, S-A/.Joo, H. Park, S. Kang, S-C.Lee, C-H. Kim, S-Y. (2011). Clinical & Molecular Allergy; 9. 1476-7961 doi 10.1186/1476-7961-9-4. >
7. Lin, CC. Lin, JM. Yan, JJ. et al. (2010). Anti-inflammatory and radical scavenge effects of Arctium lappa. Am J Chin Med; 24: 127-137. >
8. Yarnell, E. Abascal, K. (2010). Herbal medicine for viral hepatitis. Alternative & Complementary Therapies; 16(3): 151-7 doi: 10.1089/act.2010.16308 >
9. Lin, SC. Lin, CH. Lin, CC. Lin, YH. Chen, CF. Chen, IC. Wang, LY. (2008). Hepatoprotective effects of Arctium lappa on liver injuries induced by chronic ethanol consumption and potentiated by carbon tetrachloride. Journal of Biomedical Science. 9 (5), 401-9. >
10. Mie, S. Lee-Kim, ES. Hwang, S. Kyung, HK. (2009). Extraction, Partial Characterization, and Inhibition Patterns of Polyphenol Oxidase from Burdock (Arctium lappa). Enzymatic Browning and Its Prevention, Chapter 21, pp 267–276, doi:10.1021/bk-1995-0600.ch021 >
11. Burdock (Arctium lappa): MedlinePlus Supplements. Nlm.nih.gov. 2011-07-20. http://www.nlm.nih.gov/medlineplus/druginfo/natural/patient-Burdock.html. >
12. Burdock Leaves. An Innovative Burn Treatment. http://morechristlike.com/Burdock-leaves/. >
13. Ann Harbor Center for Holistic Health & Wisdom holisticwisdom.org/hwpages/firstaid.htm >
14. Leininger, M. (2004). Culture Care Diversity and Universality: A Theory of Nursing. p 95. Sudbury, MA: Jones & Bartlett Publishers. >
15. Sitzman, K. Eichelberger, LW. (2010). Understanding the work of nurse theorists: A creative beginning (2nd ed). Sudbury, MA: Jones and Bartlett Publishers. >
16. Weyer, SM. Hustey, VR. Rathbun, L. Armstrong, VL. Anna, SR. Ronyak, J. Savrin, C. (2003). A look into the Amish culture: What should we learn? Journal of Transcultural Nursing; 14(2): 139-145.